Dr. Joseph Cacchione Drops Weight Loss Drug Coverage: GLP-1 Costs Too High for Employers
Dr. Joseph Cacchione, a CEO, stopped covering GLP-1 weight loss drugs like Ozempic for his employees because the costs became too high. Many other employers are making the same decision as more workers use these expensive medications.
Dr. Joseph Cacchione made a tough choice that many CEOs are facing: he cut coverage for GLP-1 weight loss drugs because his company could no longer afford them.
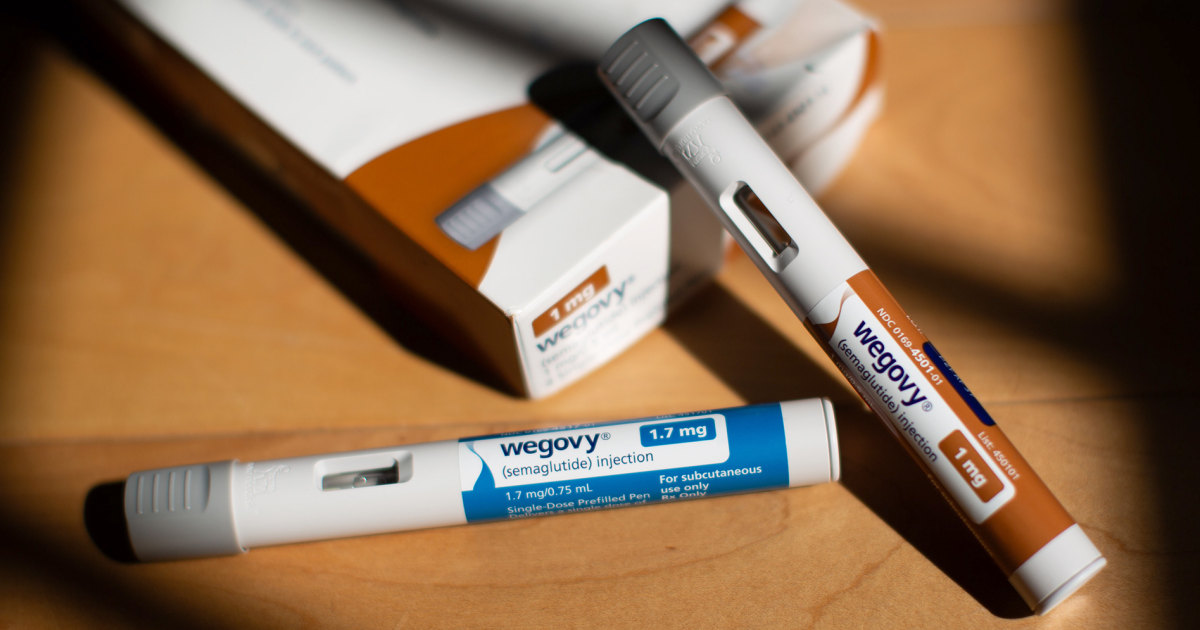
GLP-1 drugs include popular medications like Ozempic and Wegovy that help people lose weight. They work well but cost over $1,000 per month per person.
A new survey shows many companies are dropping coverage for weight loss drugs entirely. One employer in the study said they now "exclude weight loss, the entire anti-obesity category" because too many workers started using the drugs.
The Kaiser Family Foundation warns that GLP-1 drug costs could drive up health insurance premiums for everyone next year. "There is a quiet alarm bell going off," said Drew Altman, the foundation's CEO.
Drug maker Eli Lilly is trying to help by partnering with telehealth companies to make the drugs easier and cheaper for employers to offer. But for now, many workers are losing a benefit they've come to depend on.
The trend shows how successful new treatments can backfire if they become too popular too quickly for insurance systems to handle.
If you get health insurance through work, you might lose coverage for popular weight loss drugs that cost over $1,000 per month. This could mean paying thousands out of pocket or going without treatment that many people rely on.
Watch for health insurance premium increases next year as GLP-1 drug costs spread through the system.
Was this article helpful?
0 people found this helpful